Inroads into rural and remote area dementia training
- ajdc
- DTA
- education and training
- Journal Club
- rarft project
- rural and remote area dementia training
- The Rural and Remote Field Trip
- training
- Workshops
"The RARFT project brought DTA closer to rural and remote audiences, raising awareness of DTA as an organisation and promoting DTA’s dementia-specific services."

Dementia Training Australia (DTA) staff recently drove some 7500km to conduct workshops in 34 towns in rural and remote areas of all states and territories as part of DTA’s commitment to bridging the gap in dementia training between health professionals working in urban areas and their rural and remote counterparts.
The Rural and Remote Field Trip (RARFT) Project was developed as a way to engage with rural and remote health providers and workers involved in dementia care to determine and better understand their specific training needs. RARFT also provided a means to establish and grow relationships with key contacts in residential aged care, community care and hospitals in the areas visited. These project goals align with DTA’s vision that all people with dementia, regardless of service type and location, receive high-quality, evidence-based care that supports and enhances their wellbeing.
Place visited
DTA staff from Queensland University of Technology (QUT), the University of Wollongong, La Trobe University and the University of Western Australia hubs embarked on 14 field trips between June and September 2018, reaching 480 people. Towns visited were selected on the basis of having a hospital and/or aged care service, other towns within a 200km radius to maximise potential reach, and degree of remoteness (See Map)
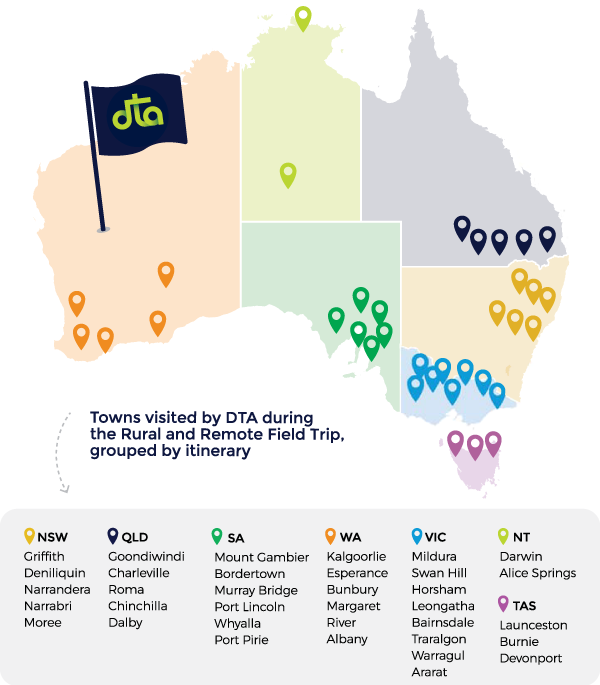
Town workshops
The half-day workshops held in the 34 towns were designed as information exchange meetings. They included a two-hour dementia education session and a discussion of training needs. The range of topics covered in the training session included: what makes a building helpful to people with dementia and to the staff caring for them; a wellbeing approach to dementia; positive approaches to responsive behaviours; optimising antipsychotic medication use in dementia care; and younger onset dementia. The discussion of training needs was started by DTA staff explaining the services on offer and encouraging participants to describe their dementia education needs and how the DTA services might need to be modified to meet them.
It was clear to the DTA staff who conducted the workshops how appreciative the participants were that they had taken the trouble to visit their communities. Many workshop participants commented about the importance of seeing DTA staff face-to-face:

DTA team members flying the DTA banner at Coonalpyn SA during a visit to the town to present a workshop as part of the Rural and Remote Field Trip Project. Photos: DTA
“It sends a message to us that DTA takes us, out here, seriously… .”
“It makes a difference when you have people with a lot of knowledge come and sit around and talk things over, recommend ways of managing things… and also for us to tell you what we do and some of our issues… .”
People also mentioned how important it is to build these relationships – expressing the hope that, having visited once, DTA staff will continue to return:
“It would be great if these things weren’t one-off events but were regular and we knew that we’d be seeing the same people again, building on what we’ve done today… .”
DTA Training Consultant Dr Christine While was staggered by the 49 health professionals, care workers and service providers who attended, in their own time, a workshop she delivered in eastern Victoria. “Their commitment to delivering great dementia care was evident, as was the desire for more dementia education in their area,” she said.
Participants commented on how important it is for DTA to understand what their work involves in rural and remote services. DTA Director Professor Elizabeth Beattie, who went to Darwin and Alice Springs with RARFT, said that participants described the pressing health issues they faced and the challenges of covering huge geographical areas, for example:
“There are so many other issues for people that they are more worried about out here […] dementia isn’t a big priority, you know, because diabetes and kidney disease and substance abuse are right in front of us… So more training about dementia risk factors and also about knowing how to recognise when a person is having issues that might signal dementia would be really helpful”.
One workshop attendee told of driving 10-12 hours, each way, to take a client home to country. He said that while he is prepared to travel vast distances because of the importance of the land for the wellbeing of his Indigenous clients, he would welcome dementia-specific training to enable him to provide better care and education for family carers.

Narrabri Hospital Community Health nurses Michel Trindall and Lavinia Hill and clinical nurse consultant Usha Kuthirayodan were among about 30 aged care professionals at the DTA workshop in Narrabri in June 2018. Photo courtesy The Courier, Narrabri
Survey results
In addition to the discussions, surveys of attendees captured rural and remote area training needs, priorities and preferences, as well as current dementia training practices of participants.
How participants access training
The majority of respondents (83%) reported having adequate technological capacity, bandwidth and equipment for staff to access online training, however limitations identified included the lack of appropriate spaces for training and limited internet access. Comments about accessing online training included:
“Slow and unpredictable internet.”
“Poor internet and expensive.”
“Not all staff live in town and have access to good internet.”
“Staff use their own devices to access training.”
When asked to indicate which modes of training they preferred, 88.7% of participants selected face-to-face training, and 66.3%selected online learning.
In reality, respondents described accessing training in a range of ways, the majority (72.7%) online (including, webinars and MOOCs), but also, for example, face-to-face (24%) and by external providers (conferences, seminars and workshops) (16.5%).
The participants were concerned about the lack of training opportunities and described many obstacles to accessing training, eg the distance to travel for training and the time it takes, being able to release staff and find a replacement, the cost of the training and the payment of the staff for their time. Comments included:
“Need to travel long distances.”
“Face-to-face usually includes travel but staff shortages limits time off.”
“Travel approx. 2-5 hours.”
“Difficult to release staff to travel.”
There were also comments on the reluctance of some staff to attend training and the expectation that staff access training in their own time:
“Not all staff are willing to train in their own time – [they] often want to be paid for training time.”
“Most staff [are] reluctant to attend training even when offered in-house, free and paid. The same staff attend and those that really need to attend don’t.”
Specific learner needs and diverse populations
Almost all respondents (99.6%) indicated that they had specific education needs related to at least one diverse population group in their area. This was most frequently Indigenous populations (36.8%), and Culturally and Linguistically Diverse (CALD) populations (33.7%) (see Table 1).
Specific education needs identified in the ‘Other’ category related to a range of characteristics of clients, often compounded by issues of isolation. For instance, issues unique to farmers and people living on the land in rural/remote areas were raised. One person observed: “Country people are independent and are reluctant to seek assistance until dementia is well advanced”.
| Population group | % |
|---|---|
| ATSI | 36.8 |
| CALD | 33.7 |
| Veterans | 29.1 |
| Younger onset | 28.8 |
| LGBTI | 13.7 |
| Homeless | 11.2 |
| Other | 7.7 |
Single people/people living alone, financially disadvantaged/lower socioeconomic status, travellers/grey nomads and people with acquired brain injury were all identified as groups with specific needs that presented specialist training requirements for health professionals. Training in how to engage with the community, such as “raising awareness amongst shopkeepers” was also identified.
What else does DTA need to know?
In response to the question, “Is there anything else we need to know specific to your geographic location and size?”, the diversity of the population was again raised. Groups specified were Indigenous and farming communities, an ageing population and multicultural communities.
Respondents talked about the large geographical areas that they had to cover. Some who worked in community-based care used the term ‘spread-out’ to refer to the health service (“a large area with a spread-out health service”) and to the location of clients. With spread-out health services it was observed that there are limited professionals available for advice and visits. Another commented that they “cover half of NT remote communities – some with phone access, some not”.
Challenges accessing training because of the distance to travel were exacerbated by insufficient staff numbers and, in some cases, size of facilities or capacity of providers to provide cover:
“Low staff numbers – rostering needs to allow staff to attend.”
“Stand-alone community organisation – limited funds.”
AJDC and the Journal Club
As part of the RARFT project, DTA also contacted 172 of the most remote services in Australia, identified from Department of Health records, and provided them with a complimentary 12-month subscription to the Australian Journal of Dementia Care, along with a Journal Club Discussion Guide. The guide was designed to encourage team discussions about the needs of people with dementia and care practice, using ideas raised in key articles in each issue of the journal. DTA also invited these services to complete its training needs questionnaire on their special circumstances and needs.
RARFT learnings and outcomes
The RARFT project brought DTA closer to rural and remote audiences, raising awareness of DTA as an organisation and promoting DTA’s dementia-specific services. As a result, a number of organisations are entering into DTA Tailored Training Packages (TTPs) and more DTA workshops are being scheduled in rural areas, including some already held in a number of the towns visited. DTA will continue to communicate with more than 600 rural and remote health professionals, care workers and service providers reached through the promotion of the trips and the connections made with those who attended the workshops.
For RARFT Project Manager, Sandra Jeavons, the opportunity to travel to rural and remote western Queensland and talk to health professionals in their environment provided many insights. “Getting out there and hearing the stories about how they provide care for people with dementia and the barriers they face each day has been invaluable.” What DTA learnt through the three months on the road will inform future strategies and has already made some inroads into bridging the rural-metropolitan gap in dementia education.
Authors
Acknowledgement
The RARFT project was a national DTA collaborative project led by the QUT team who would like to thank everyone involved in making the project a success.
To follow up on this article contact Sandra Jeavons at dta@qut.edu.au and for information on DTA visit www.dta.com.au

